Being told you need a graft of any kind – skin, bone, soft tissue – can be daunting. It sounds like a long and painful process. But with dental bone grafting, that’s simply not true. Grafting the jaw bone to reinforce and restore its integrity is a fairly simple procedure; it’s relatively painless, and recovery happens in a few days. And now, with our Smart Dentin Grinder® technology, there’s a more holistic and effective way of grafting your jaw bone.
However, no matter how state-of-the-art our method of creating and applying grafts to the jaw bone is, there is still healing time involved, where the patient’s bone integrates with the graft, resulting in stronger, denser bone tissue in the grafted area. Let’s talk about the details of dental bone grafting. You’ll realize, it’s not as scary as you might think.
10 Questions About Dental Bone Grafting Answered
Here are 10 of the most common questions patients have about bone augmentation in the jaw and how we perform dentin grafts at our Wilmington office:
-
What is bone grafting for the jaw?
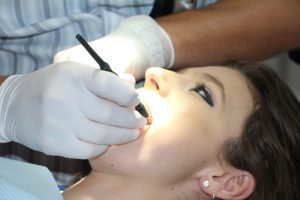
Dental bone grafting is when an oral surgeon cuts into the gum to expose an area of the jaw that has deteriorated, attaches boney material (the graft) where two pieces of bone need to bond, applies a supportive material like a dissolvable adhesive, and closes the gums back up. The surgery itself doesn’t take long, and the pain afterwards isn’t any more than a typical tooth extraction.
There are 3 main types of dental bone grafts:
- Block bone grafts: In this procedure, most often the graft material is taken from the back of the jaw, near where your wisdom teeth are/used to be. This grafting procedure is used for jaw supplementation in cases where there is significant bone loss near the front of the mouth.
- Sinus lifts: If your upper jaw has deteriorated near the back of your mouth, your sinuses can fall, creating ear, nose and throat complications. This graft supplements the lost bone to move and secure the sinuses back where they belong.
- Socket grafts: These are simple little dental grafts placed into an empty socket after a tooth extraction to counteract the natural bone deterioration that happens to an empty socket.
-
Why does someone need a dental bone graft?
There are several procedures which may require oral bone grafting to restore or preserve the health of the jaw, and for any subsequent procedures to be effective. These might include:
- Reinforcing the jaw in an area of severe deterioration from missing teeth
- Supplementing bone tissue removed during an impacted wisdom tooth extraction
- Reinforcing bone matter in an empty socket to prepare for dental implant surgery
-
What’s a jaw bone graft made of?
There are several sources an oral surgeon might use for a dental bone graft:
- Dentin Grafting: The oral surgeon extracts a tooth from somewhere else in the patient’s mouth, grinds it up, reconstitutes it and applies it as an autologous dental graft.
- Autografts: Bone tissue is sourced from the patient from somewhere else in the body. This is the ideal method of replacing lost jaw bone tissue, because a graft made of the patient’s own tissue can’t cause rejection responses from the immune system.
- Allografts: Bone tissue is sourced from another person (typically cadavers).
- Xenografts: Grafting material is sourced from a biocompatible animal (usually cow). Xenoplasts are more likely to result in failure and/or long-term complications.
- Alloplasts: Graft source is a non-living natural or synthetic material. This is most often used in extensive facial reconstruction procedures where it’s simply unrealistic to install such a large amount of live-bone dental grafting.
Our oral surgeon performs bone grafting using the dentin method. It’s holistic, sustainable, and the peak of biocompatible because the source of the bone graft is from the patient’s own tooth. This is highly preferred to autografts, which were previously the “best” choice for dental bone grafts. However, taking a piece of bone from somewhere else on the body means one more procedure, another uncomfortable recovery, and higher oral surgery costs. The Smart Dentin Grinder® recycles tooth tissue, reducing waste, eliminating the need for a surgery to harvest the autograft, and speeding procedure, healing and osseointegration time.
-
What’s involved in healing, and how long does osseointegration take?
You’re under for the procedure, and actual discomfort is minimal, especially if you didn’t have to have bone tissue taken from your hip to make the graft. We’ll tell you to take it easy for a few days, not to use straws, etc.: the typical aftercare we’d recommend after a simple tooth extraction or wisdom tooth removal.
You’ll likely only need OTC painkillers for a couple days, but we do provide prescription painkillers in limited amounts for patients who are in greater discomfort than they had expected. You’ll also be given a course of antibiotics to prevent infection. Because the jaw bone graft is under your gums, it’s not easy to see an infection forming, like you could with an above-the-gums procedure. A short course of gentle antibiotics ensures you don’t have to worry about this.
Osseointegration, or the process of your jaw bone integrating with the graft, is something you don’t feel, and it occurs over anywhere from a couple months to 6 months or more. It all depends on the patient: age, physical health, extent of damage, and extent of restoration needed.
-
What complications might happen with a bone graft in the jaw?
With proper aftercare and monitoring, there are rarely complications from a dental bone grafting procedure, especially if it’s autologous. With dentin grafting and autografting, there’s nearly no risks besides the graft simply not taking. Infrequent but possible side effects, usually brought on by adverse physical health and healing processes in the patient, include:
- Blood clots
- Complications with anesthesia
- Rejection
- Infection
- Nerve damage
- Exposure of the jaw bone graft
-
Who is most at-risk for complications from a dental grafting surgery?
Some people have a higher risk of a dental graft partially or totally failing, and they have to do with both health and lifestyle factors:
- Immune disorders
- Certain medications
- Diabetes I and II
- Obesity
- Advanced age
- Osteoporosis
- Excessive alcohol consumption
- Drug use
- Smoking
This is why it’s so important to thoroughly discuss your medical history and current health status with our oral surgeon. It informs us on how to create the best plan that keeps you safe and optimizes the chances of the graft integrating with your jaw.
-
How does your Cincinnati oral surgeon perform dental bone grafts?
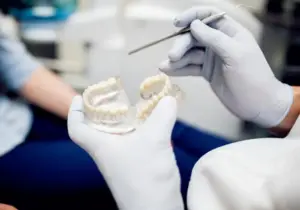
We use dentin grafting as our preferred method of jaw bone grafting. It’s a state-of-the-art, holistic method of sourcing grafting material. Our oral surgeon will take an extracted tooth and run it through the Smart Dentin Grinder®. This machine grinds the tooth up into fine particles that are cleaned, made inert, and then applied to the site. It takes less than 10 minutes to generate the graft, all right here in our office!
This method of bone grafting for jaw restoration has several benefits, including increased rates of success and healing time regarding the osseointegration. Since there are living cells in the graft, the body immediately starts pulling resources towards the graft once it’s applied. Also, most of the time, we don’t need all the graft material we created, meaning we can save the extra material should you need more dental bone grafting down the line.
-
What are the advantages of dentin bone grafts?
Dentin grafting has changed the “face” of bone grafting for the jaw. It’s increased the number of patients who have successful osseointegration; it’s reduced healing time, which also means reduced time for the dental implant process; and it’s allowed our oral surgeon to efficiently create autografts from recycled material in a way that doesn’t interfere with the patient’s body.
And as patient comfort, cost management, and efficient treatment are our main foci for every patient we see, the process of getting a dental bone graft at our Cincinnati oral surgery practice is a breeze.
-
What’s the aftercare like for jaw bone augmentation?
Since what’s going on is under the surface, caring for a healing dental graft is pretty simple, as your oral surgeon will have already stitched the site up for you after installing the graft. After that, it’s pretty much like taking care of the site of a tooth extraction – be gentle and be mindful.
We’ll give you detailed instructions on pre- and post-op at-home care, and we’ll also prescribe the StellaLife VEGA Oral Care Recovery Kit® – a 10-day holistic approach to oral surgery healing and pain management.
You should stay away from hard foods the first week, refrain from anything that makes you strain in the face and neck, avoid straws, and follow any aftercare instructions we’ve given you. It’s best to avoid any type of tobacco use when dealing with an oral surgery – even if this is one you can’t see, smoking can still delay or stop it from healing.
-
Where can I find an oral surgeon who uses dentin grafting?
Right here at Wilmington Oral Surgery! Dentin grafting is an extremely useful advancement in jaw grafting technology, and helps us make our patients’ health, surgeries and experience better, safer and more effective. Have more questions about dental bone augmentation or what’s required before you can get dental implants? Give our office a call and schedule an appointment with our oral surgeon for an evaluation.