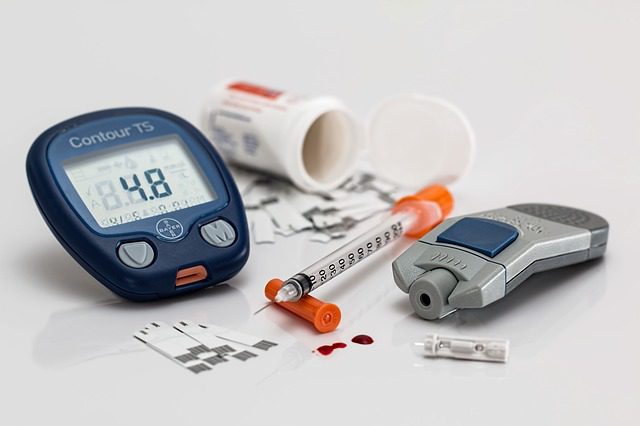
Nearly 30 million Americans have a form of diabetes, most of whom have Diabetes Type II. Those with Type I can do little but manage the condition, whereas Type II, if brought on by unhealthy lifestyle, can be reversed. The issue is, people don’t understand all the risks Diabetes II brings with it. This disease can damage a number of parts of your body, and your mouth is one of them.
Unfortunately, many do not know that diabetes comes with an increased risk of gum disease, oral infections and tooth decay. People with diabetes are at risk for serious gum disease because they are more susceptible to bacterial infections, and have a lower ability to fight the bacteria that invade gums.
In addition to the low white blood cell count that reduces immunity, people with high blood sugar have more sugar in their saliva. Since your body produces saliva to help strengthen your enamel, the high sugar content in a diabetic’s saliva can render it useless, and your teeth more susceptible to the acids sugar produces.
Gingivitis & Periodontitis Indications
Plaque-induced gum disease (gingivitis) is a bacterial infection. The gums become red, swollen and may bleed. Plaque not removed by brushing and flossing hardens to form tartar that brushing can’t remove. If the disease is not too severe, we treat it with chlorhexidine rinses and fluoride toothpaste. Once the infection has progressed, antibiotics may be needed to kill the bacteria.
Periodontitis is the name for advanced gum disease; it develops when gingivitis is not treated. The gums pull away from the teeth and form pockets that harbor bacteria. As periodontitis progresses, the jaw begins to deteriorate, causing the bone and connective tissues break down. This can result in additional infections and cause other teeth to shift. The tooth may eventually become loose and have to be pulled.
Gum Disease & Diabetes: Why it’s Different
Gum disease and glucose control seem to have a reciprocal connection. Not only are people with diabetes more susceptible to developing gum disease, but serious gum disease can then affect the ability to control your glucose levels and hasten the progression of diabetes. So while anyone can develop gum disease at any time, people with diabetes have to be even more diligent about their oral care than the rest of us.
As a result of this uphill battle, over 20% of people diagnosed with diabetes suffer from gum disease at some point in their lives; the feedback loop of chronic oral infection and glucose control can be difficult to manage. Gum disease is also associated with developing heart disease, adverse pregnancy outcomes, and a host of other health issues. That’s why prevention and early treatment are paramount.
Preventing Gum Disease: Pay Attention to Your Mouth
While gum disease can be treated, it is far better to prevent gingivitis from progressing to periodontitis in the first place. And it’s not that difficult; it just takes a little attentiveness and a lot of the better-safe-than-sorry philosophy. It isn’t always easy to tell if you have gum disease; you might not have any pain. But there are some warning signs:
- Gums that bleed on their own or when brushed
- Gums that are red, swollen or tender
- Gums that seem to be receding, especially if you start to see the darker parts of your tooth at the gum line.
- Chronic bad breath
- A bad taste in your mouth
- Teeth that seem to shift, don’t seem to fit together when you bite, or partial dentures that aren’t fitting properly
- Loose teeth
If you have been told you have gum disease, or think you might, we would be happy to provide a second opinion. Preventing gingivitis, gum disease and periodontitis is all about staying on top of your oral health, so talk to an oral surgeon or two if you notice anything weird about your mouth, whether teeth, gums or jaw.
Another Reason to See Your Dentist Twice a Year
Plaque control is critical to preventing gum disease, as plaque and tartar buildup at the gum line is where the bacteria hides and proliferates. Get a professional cleaning twice a year, and use any prescription toothpastes, mouth rinses or antibiotics your oral specialist prescribes.
During your regular checkup, your dentist or hygienist will scrape away the plaque and tartar (hardened plaque) above and below the gum line. Yearly x-rays are also a must, especially if your gum disease is advanced. If you have early signs of gum disease, your dentist may ask you to schedule cleanings more than twice a year.
Other Oral Complications with Diabetes: Thrush & Dry Mouth
Thrush, an infection caused by fungi that grow in the mouth, and dry mouth, which can cause soreness, ulcers, infections and cavities, are also associated with diabetes.
Thrush is a risk because fungal infections thrive off of sugars, and people with diabetes have high sugar levels in their saliva. This, coupled with the compromised immunity and frequent antibiotic intake all create the perfect environment for yeast and fungal issues. Signs of oral thrush include:
- Corners of your mouth become dry, red and cracked
- Feeling of dry mouth
- Inability to taste
- Irritation and pain under your dentures
- Redness, burning and pain when chewing
- White patches on the tongue and gums; can be creamy or lumpy
Dry mouth is another oral complication people with diabetes are disproportionately susceptible to. This is because diabetes reduces saliva production. Dry mouth leaves you at risk for tooth abscesses, infections, mouth ulcers, and tooth decay. Signs of dry mouth include:
- Chronic bad breath
- Chronic sore throat
- Nose feels dry on the inside and may bleed
- Problems tasting
- Problems with your dentures
- Sores in the mouth or on the lips and tongue
To prevent these maladies, blood glucose control is critical. Avoid smoking, and if you wear dentures, remove and clean them daily. Practice excellent oral care by brushing and flossing every day. See your dentist twice a year, unless you are advised to visit more often. In addition, a healthy, nutrient-filled diet and an active lifestyle can strengthen your body’s defenses, as well as help other health issues. If you have Diabetes II, the right lifestyle changes might even cause the condition to go into remission.
Partner with your Oral Care Team to Keep Your Smile Healthy
To ensure appropriate oral care if you have diabetes, keep your dentist, hygienist and oral surgeon informed about your condition and the medications you take. Stay in close contact with the doctor who manages your treatment plan; well-controlled glucose levels are key. You may have to postpone non-emergency dental procedures when your blood sugar is out of control, and that could leave more time for gum disease to progress. Help us help you, and you can have a beautiful smile and a healthy mouth without having to undergo several oral surgeries and be on constant medications.