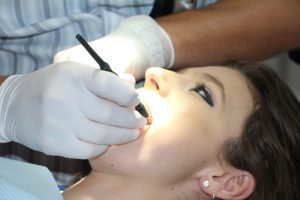
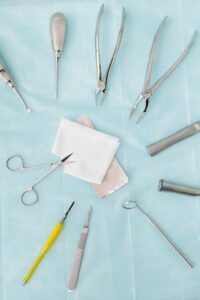
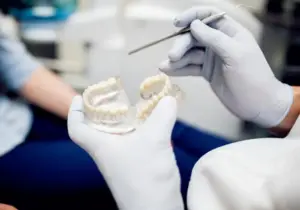
I first began my career as an oral surgeon with a group practice — to which I dedicated the first 6 ½ years of my career. Like many oral surgery offices, this group was enrolled in multiple dental insurance plans. I assumed this approach had the best interests of my patients in mind. Why fix what’s not broken? I was a young, energetic oral surgeon — my passion was treating patients, not bureaucracy.
At that time, I had no idea my patients were systematically being ripped off by an industry that only saw them as a line item on a spreadsheet. Hindsight is keener than a digital x-ray.
What I Learned Launching My Own Practice
As my career evolved, I launched my own solo practice at the end of 2006. Suddenly signing up for insurance plans as an in-network provider was personal. This was my own practice, after all. It was my name on the door. I wanted the very best for my patients.
Being overwhelmed with launching a new practice, I started with the traditional playbook: I signed up to be a network provider for all of the major dental insurance companies and some smaller providers.
My office manager labored through all the rote paperwork as my practice evolved over the next few years. She hoped I would not see the amount of write-off we had to absorb as an in-network provider, or the scam insurance companies routinely played on my patients as a business prerogative — ripping them off under their very eyes.
As time went on, I grew tired of seeing my patients ripped off by the disreputable practices of the insurance industry. I knew there had to be something better — alternatives that could save my patients money while simultaneously providing higher quality care.
Diagnosing the Insurance Industry: What We Discovered
To document the numerous ways insurance companies routinely bilked patients, I mapped a chart on the back of large cardboard box listing every dental insurance company on my docket, noting:
- Common Procedure Codes
- The Fee Schedule & Recommended Fee for Each Procedure
- Our Fee (always lower than the recommended fee)
- The Insurance Payment
- The Amount & Percentage of Write-off from our Fees
The results were eye raising and shocking. These charts profoundly changed how I approach fees and the insurance companies I work with. This has resulted in better care for my patients at more affordable rates.
Think about the uninsured and under-insured — a significant portion of the population. Both are unfairly abused by the system. Those with no insurance bear the full brunt of the cost; those with some coverage get the same work done at a 35-55% discount. Both are ripped off and played by an unscrupulous insurance industry.
The following examples are true — they are not hypothetical. Like a 3-card monte scam, the insurance industry gets away with overburdening patients through a sleight of hand. They do not want the patient to be informed or the sheer con would be too obvious. An unaware patient is much easier to control and manipulate. Profit drives their every motive — not patient care or well-being.
Dental Industry Tactics: Real Life Examples of Predatory Practices
The dental insurance company is not your friend and is not looking out for your best interest. Their job is to maximize profits for the insurance company by delaying payments and not paying claims.
- Knowing this, it is not surprising that some dental insurance companies have a tendency for some of the most commonly used codes, such as the code for a surgical extraction (D7210), not to be covered. Therefore, the patient has to pay and the insurance company saves money.
- Anesthesia is rarely covered for the removal of primary (baby) teeth. A few will cover anesthesia if 10 or more baby teeth are removed at one time. Note that there are only 20 baby teeth in total. The insurance company routinely does not care if the teeth are infected or causing pain. Performing many of these procedures with only local anesthesia in kids is a perfect way to make a severe dental phobic patient for life.
- Only a few of the dental insurance companies will consider covering sedation for the removal of one or two teeth, and these teeth need to have significant issues to be able to fight for coverage. If the provider is out-of-network, the dental insurance company will demand medical to process the claim first or receive a denial of coverage from the medical insurance, as a delay tactic.
- When there are three or more teeth to be removed, some companies mandate that the teeth are in different areas of the mouth for anesthesia coverage. If the teeth are all in one quarter of the mouth, anesthesia may not be covered.
- Insurance companies have been known to change the procedure code. They tell the provider and patient what the plan should be without ever looking in the patient’s mouth or examining the situation. The patient and provider have no recourse to change this mandate.
- Insurance companies will, at times, deny coverage for work done. This sometimes occurs despite prior confirmation of coverage and legal obligation. Certain insurance companies will not cover wisdom teeth unless proven to be a medical necessity. They also will deny the first appeal, only to relent with a second appeal. The insurance company knows that most patients and dental offices will give up with either the first or second denials. If this time exceeds a year in duration, the insurance company will close the claim and refuse to pay. Again, this saves the insurance company money.
- Most dental insurance plans are PPO plans, which mean that the patient can still see any provider they desire and have the same benefits of coverage for dental work. We have seen that the in-network and out-of-network percentage coverage is the same for nearly all of the companies. A small minority of the plans have significantly lower coverage for out-of-network providers, and we inform the patient of this before providing any treatment.
- Even with a PPO plan, the insurance company tells patients that they must see an in-network provider for coverage. This is not true.
- A small minority of dental plans are HMO / DHMO. These plans will dictate seeing an in-network dentist for any coverage. This is how they limit options for patients. As a specialist, we have seen that the list of in-network oral surgeons for some of these HMO / DHMO plans is very limited, and geographically difficult.
- Medicare rarely covers dental treatment. Patients are told by Medicare that since they are seeing us, an oral surgery office, and ‘surgery’ is involved, Medicare will cover all of the costs. However, this is not the reality. There are no out-of-network benefits for the Medicare dental plans.
- Most Medicare supplemental dental plans available are basic plans, which mean they routinely cover basic services like exams, cleanings, and x-rays. Most of these plans do not cover the treatment most patients need – extractions, implants, crowns, partials / dentures. Unfortunately, many patients are told by the Medicare person on the phone that the dental plan they are getting is excellent. Any potential benefits apply only to Medicare network providers.
- Many insurance companies will not cover bone grafting at the time of tooth removal; however, they may consider covering grafting when the implant is placed. It is far better, and less complicated, to graft the extraction site and save the bone, rather than let the bone shrink and deal with the bone loss when the implant is placed. The insurance company knows this. This is yet another way to deny coverage.
- When anesthesia is covered, for example with wisdom teeth, the insurance company allows for four 15-minute increments of anesthesia to be billed. There is rarely an instance when an oral surgeon will need a full hour to remove four wisdom teeth or for one surgical extraction; however, since it is allowed by the insurance company, many will charge the patient the full hour. Be sure to ask the expected duration of the procedure and then look at the treatment plan. The current anesthesia codes for deep sedation are D9222 and D9223. Anesthesia time only applies to the surgery itself, not the recovery time once the surgeon leaves the room.
- The ‘missing tooth clause’ relates to patients with one or more missing teeth which they desire to replace. If the tooth was missing before the patient had his/her current insurance, the missing tooth clause can come into play. The insurance will not cover to have the tooth replaced. They say it’s basically not their responsibility. If the tooth is removed while the patient has the insurance, most will cover the replacement.
- Many instances have been seen when the dental plan does have coverage for an implant; however, the insurance company will deny the implant and suggest ‘alternative treatment.’ These alternate options are inferior and are meant to save the insurance company money. This is yet another example of an insurance company dictating treatment without any clinical validation.
- The ‘waiting period’ for treatment can range from zero days to 24 months. If a waiting period is in place, the patient essentially has no coverage until the waiting period has passed. Patients are frequently not told of a waiting period or duration of the waiting period. Be sure to have the dental office contact the insurance company if you have new insurance and check on this.
- If a patient has treatment to replace teeth, perhaps a partial or bridge, which is not satisfactory for function and this was sent to the insurance company for payment, the insurance company will most likely not pay for a better tooth replacement option for up to ten years. The insurance company will state that they have already paid for this tooth to be replaced. Even if implants are covered, the patient is out of luck. The insurance company will not tell you this beforehand. The partial is much less expensive, and the insurance would rather pay for a cheap partial than a more expensive, better fix.
- At times, a pre-estimate is obtained before dental treatment. This estimate received by the patient and dental office is not a guarantee of coverage from the dental insurance company. We frequently see insurance companies state that they will review for coverage, even after a pre-estimate has been obtained.