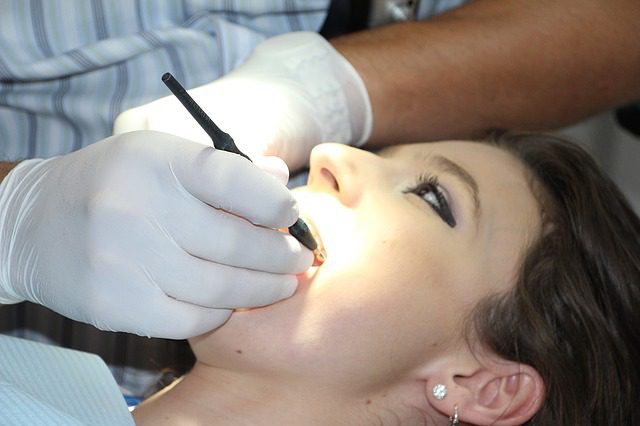
Plenty of oral surgeries require the use of dental anesthetics. There are a number of different sedatives used in oral procedures, each with its own effects on the body. Sedatives keep the patient semi-conscious, while general anesthesia puts the patient in a fully unconscious state. But what goes on in the brain while the patient is under the effects of sedatives or anesthesia during an oral surgery?
Some patients love to know the ins and outs of sedation used in dental surgeries, and this post is absolutely for them. Knowledge is half the battle, and in this case, it helps reduce dental anxiety surrounding sedatives.
The Spectrum of Consciousness During Oral Surgery Sedation
When patients come in for surgery, they’re put under what is referred to as “conscious sedation.” It’s a drug-induced state of consciousness where patients are incredibly relaxed. They’re still able to respond with intention to verbal commands, and they maintain their breathing and other natural reflexes. Oral sedatives used in dentistry are considered highly safe for patients.
General anesthesia used in mouth surgeries, however, is different. When a patient is put under general anesthesia, they’re completely unconscious. They require a machine to help them breathe, and they have no protective reflexes. General anesthesia is used in only the most complicated cases. IV sedation during oral surgery is used for maximum patient comfort, and it maintains crucial bodily functions.
When a patient is given an oral sedative before a dental procedure, the effects kick in quickly. Patients feel deeply relaxed and drowsy, and they experience a significant reduction in anxiety. Their time perception is slightly skewed, and time passes quickly.
How Dental Sedatives Work
Oral surgery sedatives work by repressing the GABA system in patients’ brains. The GABA system is a neurotransmitter located in the brain. Its main function is to slow down nerve cell communications, preventing overstimulation. In short, it reduces stress and anxiety, and it promotes relaxation. If this sounds familiar, it’s because that’s essentially what dental surgery sedation does. IV sedatives for oral surgery work in tandem with the GABA system and enhance its effects. With the help of a sedative, the GABA system slows down the transmission of signals between neurons. This suppresses awareness and slows thoughts.
Dental surgical practitioners go through rigorous training for sedative administration. They’re expertly trained to slowly adjust the dosage to achieve maximum effect with minimal risk.
Why Amnesia is a Common Side Effect of Dental Sedation
It would be tough to find someone who wants to remember their surgical dental procedure. Thankfully, one of the most common effects of sedatives is the ability to cause amnesia in patients. During dental IV sedation, the ability to form new memories is greatly inhibited. Patients might remember bits and pieces, but most of the operation is a blur.
The hippocampus is a familiar region in the brain to most. It’s the region that converts short-term memories into long-term memories. The sedatives commonly used in dental surgeries disrupt the hippocampus and its functions. This disruption prevents the formation of new long-term memories, a concept known as anterograde amnesia. This is actually a huge win for patients—they avoid the mental trauma and anxiety that comes along with the sights, sounds, and feelings of a dental operation.
The Safety Net for Dental Sedatives
The sedatives routinely used in oral surgeries are incredibly safe and effective. However, there’s always the potential for a unique patient reaction to the medication or a complication. In the event of complications, there’s a reversal agent for IV dental sedatives. Flumazenil is the most commonly used reversal agent in oral surgeries. The drug rushes to the same GABA system receptors as the sedative. The reversal agent pushes the sedative molecules off the receptors, immediately restoring the normal function of the GABA system.
Dental surgical specialists rarely have to use a reversal agent. The most common circumstances that necessitate a reversal agent are:
- Paradoxical reaction to dental sedatives – Sometimes, patients experience the opposite of calm after taking a sedative. They might become aggressive, displaying agitation and confusion.
- Respiratory depression – If the patient’s consciousness levels fall too low, their breathing slows. The reversal agent immediately restores their normal breathing abilities.
- Unforeseen emergency – If a medical event unrelated to the sedative arises, reversal agents immediately wake up the patient. This allows them to be fully cognizant for further diagnosis and treatment.
The entire sedation process during a dental operation is managed by trained professionals. The dental surgeon and their assistants are highly competent and focused on safety and comfort. The biggest, most exciting memory of the day will be the car ride home, guaranteed.